
TENACIOUS SUPPORT DURING THE COVID-19 PANDEMIC
When Diana got pregnant last fall, there was no coronavirus in Pennsylvania. Nobody was talking about quarantines or social isolation.
Diana, who lives in Lancaster, was thrilled and a bit apprehensive because a previous pregnancy had ended in a miscarriage.
Marlisa, her nurse from Nurse-Family Partnership® at Penn Medicine/Lancaster General Health, met her at her home in late-October and talked to her about her anxiety and severe nausea and how to manage them with diet, lifestyle changes and medication from her doctor.
“She was really uncomfortable,” NFP nurse Marlisa said, “but she was committed to making this pregnancy work and we both were crossing our fingers that it would go well.”
The baby was due around April 10, and Diana was excited and happy, despite the nausea.
The 27-year-old mom speaks Spanish primarily and she and her husband live with his family in a supportive multi-generational household. At the time she met Marlisa, a fluent Spanish speaker, Diana was very involved in activities at her church, planning a baby shower and eagerly looking forward to becoming a mom.
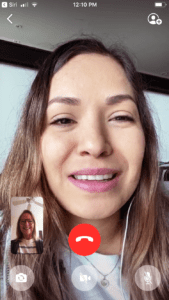
The Telehealth visits by video have been critically important-maybe even life-saving.
Then, just before the COVID-19 pandemic hit and in-person home visits were no longer possible, Diana experienced dangerous complications.
“Diana texted me one day in late February to say that she was itching a lot. I said she needed to contact her doctor immediately,” Marlisa said. When she did, she was diagnosed with cholestasis, a liver condition in which bile accumulates in the body and can cause severe itching.
When Diana saw her doctor on March 16, her blood pressure was high so she was admitted to the hospital and a decision was made to induce labor that day.
“I was worried for her since they were inducing early,” Marlisa said.
The induction didn’t go well and little Luna was finally born on March 19.
Diana’s blood pressure spiked the following day and she was treated for preeclampsia.
Left untreated, preeclampsia is a potentially fatal condition characterized by high blood pressure, seizures and organ damage.
“She doesn’t remember much about that day, her first day of bonding with her baby,” Marlisa said, because the medications she had to take have a lot of neurological effects.
Diana was stabilized and released, but when she went back to the clinic two days later for a checkup, her blood pressure spiked again.
When she went home, Marlisa said, “I talked to my supervisor and said that she really needed a home visit but, of course, I couldn’t.”
So, they brought her a device so she could monitor her blood pressure on her own. Marlisa was concerned because Diana wasn’t scheduled to be seen by her doctor for another month.
“We dropped it off in the late afternoon and that evening she called to say her blood pressure was really high – 180 over 108,” Marlisa said. “To test the cuff, she took the blood pressure of the others in her home and everybody else was fine, so I told her to get ready to go back to the hospital.”
Diana said Marlisa’s help “came just at the right time…When I checked my blood pressure and saw that it was very high, I called her. She took my call right away and then called the hospital so that I could go in to get the care I needed. She’s been a huge support for me.”
The doctors examined her and Diana was readmitted.
Marlisa said she and Diana talked about how dangerous preeclampsia is, “how that night she could have seized and died. She didn’t have enough symptoms to realize what was going on – no blurry vision or headache – so it was super that she got the blood pressure cuff. It may have saved her life.”
“Truthfully, I’m so grateful for her help,” Diana said.
Diana’s blood pressure was persistently elevated for three weeks, but it is gradually returning to normal and she no longer needs all the medications she had to take to control it at first.
Now, Marlisa’s phone calls with Diana usually focus on little Luna, who weighed 5 pounds, 10 ounces when she was born.
“She’s getting a bit bigger,” Marlisa said, and she can see from the video conference that she is “looking more normal and stable.” Diana has sought advice about breastfeeding and treating Luna’s diaper rash, typical questions from new moms, and things seem to be going well.
The telehealth visits by video have been critically important – maybe even life-saving, Marlisa said, but she misses the in-person interactions for which Nurse-Family Partnership is famous.
“I feel like there are certain dimensions missing in our phone visits,” she said. “It’s hard to see how a mom plays with her child when she’s trying to hold the phone at the same time.

Still, Diana is profoundly grateful for Marlisa’s continuing help.
In a recent text to her nurse, Diana wrote, “Thanks so much, Marlisa. I don’t know what I would do without you.”
She’s also deliriously happy about being a mom.
“I wouldn’t change anything that I have experienced so far with being a mother, like holding my baby in my arms and seeing how vulnerable she is, how dependent she is on me,” said Diana.
“I breathe a little differently when she’s close to me and she makes me want to give her all the love that I possibly can. My daughter is a miracle in my life and I give thanks to God for sending her to me.”

